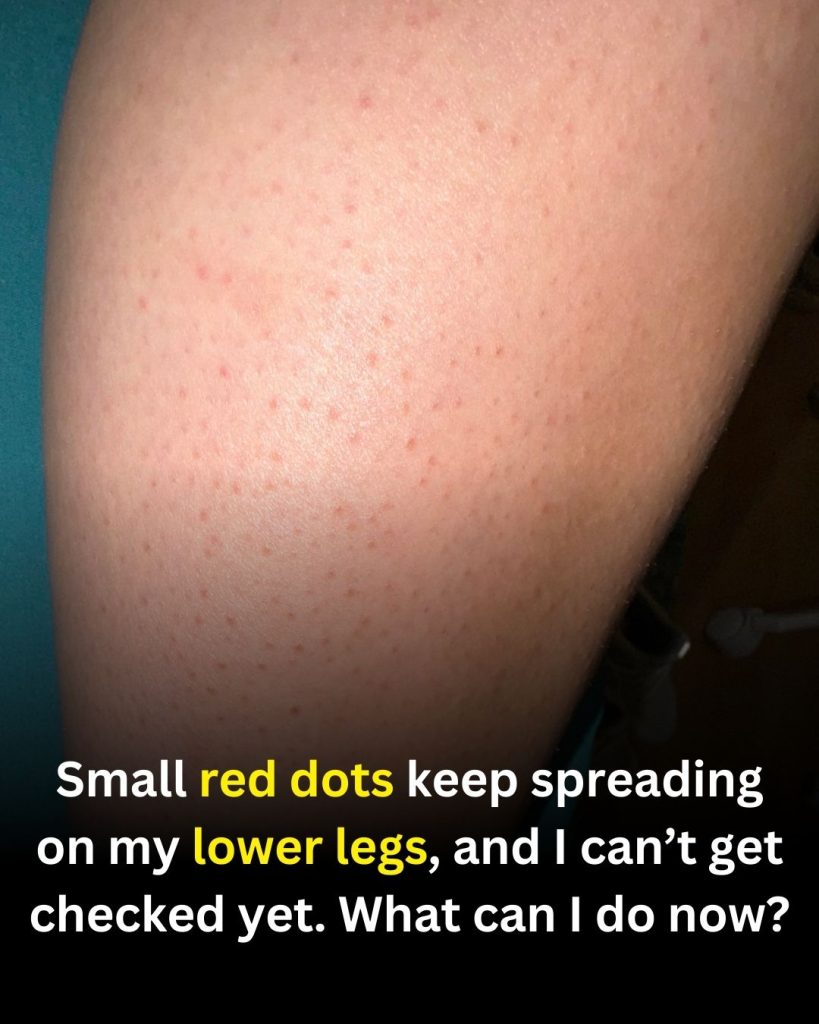
Noticing small red dots spreading on your lower legs can feel worrying, especially if you can’t see a healthcare professional right away. Skin changes can have many causes, ranging from mild irritation to conditions that need medical attention. Staying calm, observing carefully, and taking gentle care of your skin can help while you arrange proper evaluation.
This guide shares general educational information and safe self-care ideas. It does not replace a medical diagnosis. If symptoms worsen or you feel unwell, seeking medical care is important.
1) Rule Out Urgent Situations First
Seek urgent medical help if the red spots:
-
Appear suddenly in large numbers
-
Come with fever, dizziness, or weakness
-
Turn into large bruises
-
Are linked with bleeding from gums or nose
-
Follow a new medication or injury
-
Occur with breathing or swallowing difficulty
If the spots are painless, stable, and you otherwise feel fine, it is usually reasonable to monitor them briefly.
2) What Small Red Dots Can Be
One possible explanation is petechiae, which are tiny red or purple spots caused by small blood vessels under the skin. These can appear after pressure, irritation, or minor strain.
Another sometimes-mentioned cause is a mild skin condition related to tiny capillaries in the legs (often grouped under “capillaritis”). These are usually harmless but can linger.
Other possibilities include:
-
Skin irritation or allergies
-
Heat rash
-
Minor inflammation
-
Reactions to soaps or fabrics
Only a clinician can determine the cause.
3) Simple Observations You Can Do
You can safely gather helpful information:
-
Gently press a clear glass on a spot
-
If it fades, it may be surface redness
-
If it doesn’t, note it for your doctor
-
-
Track size, number, and location
-
Notice itching, pain, or swelling
-
Take clear daily photos in good light
This helps professionals later.
4) Everyday Factors That May Worsen Spots
Some habits can make leg skin symptoms more noticeable:
-
Standing or sitting for long periods
-
Tight socks or restrictive clothing
-
Heat and humidity
-
New skincare or laundry products
Reducing these may help.
5) Gentle Skin Care Steps
Safe care includes:
-
Fragrance-free moisturizer
-
Lukewarm (not hot) showers
-
Loose, breathable clothing
-
Avoiding scratching
Compression socks may help circulation for some people, but it’s best to ask a professional first.
6) Lifestyle Habits That Support Skin Health
General wellness can support recovery:
-
Light movement like walking
-
Elevating legs when resting
-
Staying hydrated
-
Balanced nutrition with vitamins C and E
-
Limiting alcohol and excess caffeine
These are supportive, not cures.
7) Over-the-Counter Options
If itchy:
-
Non-drowsy antihistamines may help
-
Mild hydrocortisone cream can calm irritation (short-term use only)
Avoid strong medicated creams unless advised by a professional.
8) Track Symptoms Before Your Visit
Keep notes on:
-
When it started
-
Changes over time
-
New foods, products, or medications
-
What helps or worsens it
Photos are especially useful.
9) Consider Telehealth
If you can’t visit in person:
-
Telehealth appointments
-
Online dermatology services
-
Nurse advice lines
These can guide next steps.
10) Red Flags That Need Fast Care
Seek prompt help if you notice:
-
Rapid spreading
-
Large bruising
-
Fever
-
Fatigue or illness
-
Bleeding elsewhere
-
Severe pain
-
Reaction after new medication
11) Advocate for Yourself
When you do see a doctor:
-
Bring photos and notes
-
Ask clear questions
-
Discuss all symptoms
-
Seek a second opinion if needed
Final Note
Many skin changes are temporary and manageable, but persistent or unexplained spots deserve medical review. Monitoring calmly and caring for your skin gently is a good first step.
If you want, you can describe itching, pain, color, and timing, and I can share general educational info — but a clinician should make the diagnosis.